

Published on March 10, 2026 By 800ZED

You are eating carefully. You are not completely sedentary. But the weight just won't move... especially around your belly. You crash hard after meals. You wake up tired even after eight hours of sleep. Your skin is breaking out, your period is unpredictable, and no matter how many times you Google your symptoms, nothing quite fits.
Here is something worth considering: it might not be your willpower, your age, or your genetics working against you. It might be insulin resistance: a metabolic condition that quietly disrupts how your body processes energy, regulates hormones, and maintains a healthy weight. And it is far more common among Filipino women than most people realize.
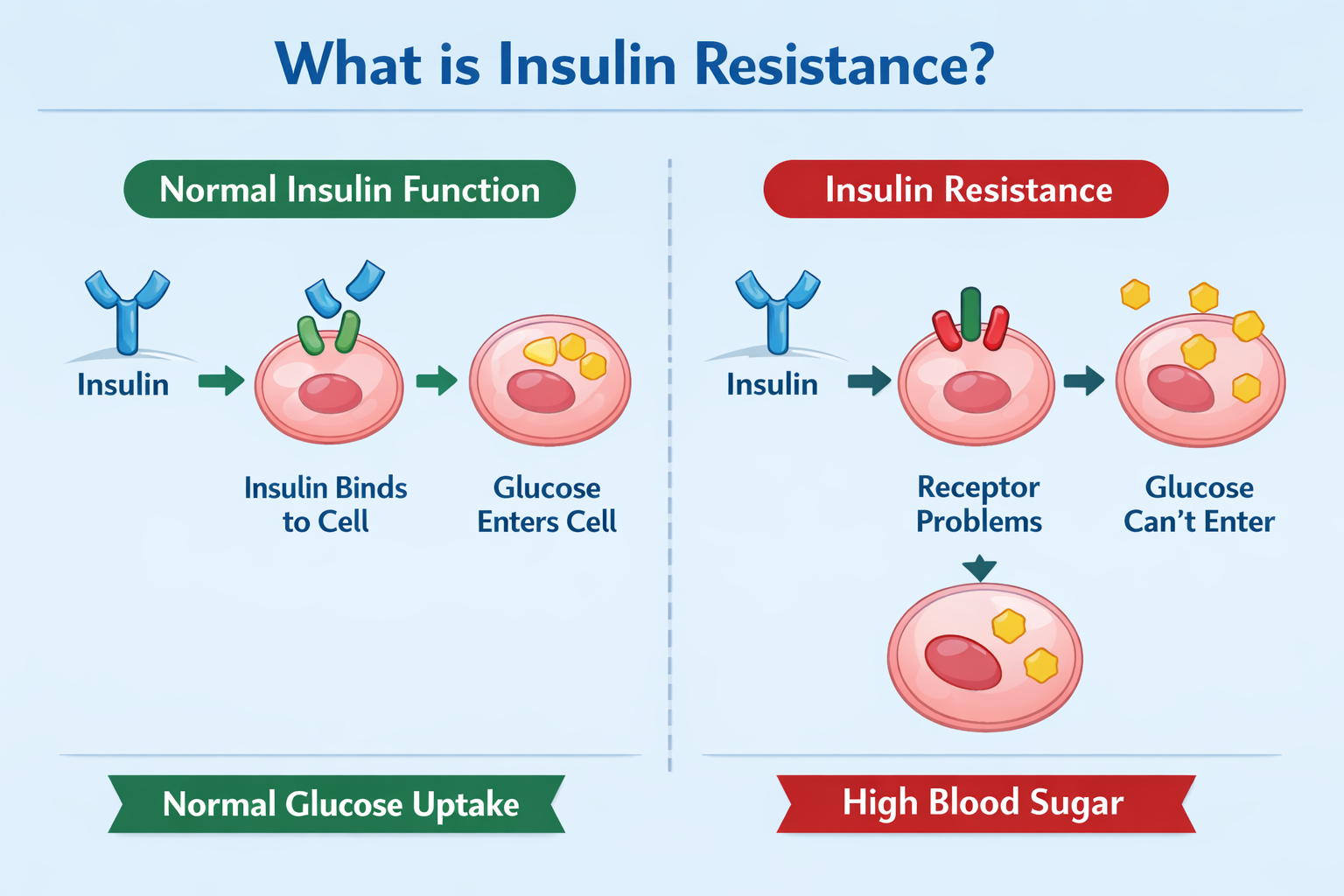 To understand insulin resistance, you first need to understand what insulin does. Every time you eat, especially carbohydrates — your blood sugar rises. Your pancreas responds by releasing insulin, a hormone that acts like a key, unlocking your cells so glucose can enter and be used as energy.
To understand insulin resistance, you first need to understand what insulin does. Every time you eat, especially carbohydrates — your blood sugar rises. Your pancreas responds by releasing insulin, a hormone that acts like a key, unlocking your cells so glucose can enter and be used as energy.
Insulin resistance happens when that key stops working properly. Your cells stop responding to insulin the way they should. Your pancreas compensates by pumping out more and more insulin to do the same job. For a while, this keeps your blood sugar in a normal range — so standard glucose tests may look fine. But underneath, your body is working overtime, and that chronic overproduction of insulin starts causing damage in ways that show up long before a diabetes diagnosis ever does.
Left unaddressed, insulin resistance is one of the most direct pathways to prediabetes, type 2 diabetes, heart disease, and a range of hormonal conditions... including PCOS. The American Diabetes Association describes it as both a precursor and an accelerator of some of the most serious chronic diseases affecting women today.
This is the part that does not get talked about enough.
Research shows that Filipino women have a higher susceptibility to insulin resistance and type 2 diabetes compared to many other ethnic groups — even at lower body weights and lower BMI levels. A study published in PMC found that Filipinas had significantly higher rates of type 2 diabetes compared to Caucasian and African American women with the same amount of visceral fat — suggesting that genetic and metabolic factors unique to Filipino women may be at play, independent of obesity.
In other words, a Filipina who is slim, active, and eating what most would consider a reasonable diet can still develop insulin resistance. The "you don't look like you have it" assumption is not just unhelpful... it actively delays diagnosis and treatment.
Add to this the reality of the Filipino diet: typically rice-heavy, with refined carbohydrates as a staple at nearly every meal, and the metabolic risk becomes even more significant. This is not about demonizing rice or Filipino food culture. It is about understanding how certain dietary patterns, combined with genetic predisposition, can quietly push the body toward metabolic imbalance over time.
This is where many women have an "aha" moment because the symptoms of insulin resistance are things they have been experiencing for years and quietly normalizing.
Fatigue after eating. Not just a little drowsy — a heavy, urgent crash that hits one to two hours after a meal, especially a carb-heavy one. Your cells are struggling to absorb glucose even though your blood sugar just spiked, leaving you running on empty.
Constant carbohydrate cravings. An intense, almost urgent need for sweets or starchy food... not just hunger, but a specific pull toward sugar and refined carbs. This happens because your cells are glucose-deprived despite elevated blood sugar, sending hunger signals even when you just ate.
just hunger, but a specific pull toward sugar and refined carbs. This happens because your cells are glucose-deprived despite elevated blood sugar, sending hunger signals even when you just ate.
Stubborn belly fat. Insulin actively promotes fat storage, particularly in the abdominal area. Women with insulin resistance often notice that weight collects around their midsection even when the rest of their body stays relatively lean. This apple-shaped pattern is one of the more reliable visual cues.
Brain fog. Difficulty concentrating, forgetting words mid-sentence, or feeling mentally sluggish... especially after meals or during the second half of the menstrual cycle, when insulin resistance naturally worsens due to hormonal shifts.
Irregular periods. High insulin levels stimulate the ovaries to produce more androgens (male hormones), which disrupts ovulation and can cause cycles to become unpredictable, longer, or absent. This is the exact mechanism that links insulin resistance directly to PCOS.
Dark patches on the skin. Darkening around the neck, armpits, groin, or knuckles: a condition called acanthosis nigricans, is one of the visible signs that insulin resistance may be present. It is caused by high insulin levels stimulating skin cell growth in certain areas.
Recurrent yeast infections or UTIs. Elevated glucose levels in bodily fluids create an environment where yeast and bacteria thrive. Women with insulin resistance are more prone to these recurring infections, though the connection is rarely made.
Morning fatigue despite sleeping enough. Overnight insulin fluctuations can disrupt the quality of sleep, leaving women feeling unrested regardless of how many hours they were in bed.
If you have already read our blog on PCOS, this will make a lot of sense.
Insulin resistance and PCOS are deeply intertwined. Up to 70% of women with PCOS have insulin resistance, and in many cases, the insulin resistance is what drives the hormonal imbalance in the first place. Excess insulin tells the ovaries to produce more androgens. Those androgens disrupt ovulation. And that disruption is what creates the irregular periods, acne, hair changes, and fertility challenges that define PCOS.
This is why treating insulin resistance through diet, exercise, and sometimes medication can dramatically improve PCOS symptoms even without targeting the hormones directly. When insulin comes back into balance, the downstream hormonal chaos often settles too.
For Filipino women managing PCOS, understanding the insulin resistance connection is not just useful... it is often the key to finally seeing real improvement.
Here is the frustrating truth: standard blood tests can miss insulin resistance entirely in its early stages. A fasting glucose test checks your blood sugar at one point in time. If your pancreas is still compensating by producing extra insulin, your blood sugar may look perfectly normal while the underlying problem is already well underway.
More informative tests include:
Fasting insulin levels. This directly measures how much insulin your body is producing, not just what your blood sugar looks like. Elevated fasting insulin in the presence of normal glucose is a classic early sign of insulin resistance.
HbA1c (glycated hemoglobin). This gives a picture of average blood sugar over the past two to three months. A reading between 5.7% and 6.4% indicates prediabetes... the stage where insulin resistance has already begun affecting blood sugar regulation.
Fasting glucose. A fasting blood glucose between 100 and 125 mg/dL signals prediabetes. Above 126 mg/dL on two separate tests suggests type 2 diabetes.
Lipid panel. Insulin resistance typically shows up in abnormal cholesterol levels — specifically high triglycerides and low HDL (good cholesterol). This combination is a reliable metabolic red flag.
Waist circumference. A waist measurement above 80 cm in women is associated with higher metabolic and cardiovascular risk, even at a normal body weight.
If you have been experiencing the symptoms above but your basic blood tests have come back normal, it is worth asking your doctor specifically about fasting insulin levels and a full metabolic panel. Advocating for yourself in that consultation could make a significant difference.
Yes — and this is genuinely good news. Unlike some chronic conditions, insulin resistance responds very well to targeted lifestyle changes. Research consistently shows that meaningful improvements can happen within two to four weeks of consistent effort.
What you eat matters enormously.

The goal is not to eliminate carbohydrates but to choose the right ones and manage how much glucose hits your bloodstream at once. Practical changes that make a real difference include:
Limiting refined carbohydrates and sugary drinks that cause rapid blood sugar spikes. For Filipino women, this means being mindful of white rice portions, white bread, sweet drinks, and heavily processed snacks... not eliminating cultural foods entirely, but being strategic about portions and combinations.
Pairing carbohydrates with protein, healthy fat, or fiber at every meal. Eating rice with fish, vegetables, and a source of healthy fat significantly slows glucose absorption compared to eating rice alone.
Prioritizing vegetables, legumes, whole grains, and lean proteins. A more diverse diet is consistently linked to better insulin sensitivity in Filipino women specifically.
Reducing pro-inflammatory foods: excessive red meat, processed food, and refined vegetable oils which worsen insulin resistance through oxidative stress and inflammation.
Movement is one of the most powerful tools available.
Exercise improves insulin sensitivity through a completely separate pathway from diet. When muscles contract during physical activity, they can absorb glucose directly without needing insulin bypassing the resistance entirely. This effect lasts for 24 to 48 hours after exercise, which is why consistency matters more than intensity.
Strength training twice a week: even bodyweight exercises like squats, lunges, and push-ups has a particularly strong effect on metabolic health because muscle tissue is the body's largest glucose sink. More muscle means more capacity to absorb blood sugar.
Moderate aerobic activity: walking, cycling, swimming for at least 150 minutes per week improves insulin receptor signaling throughout the body. Even a 10-minute walk after meals has been shown to meaningfully blunt post-meal blood sugar spikes.
Sleep and stress are non-negotiable.
Chronic poor sleep and high cortisol (the stress hormone) directly impair insulin sensitivity. A body that is sleep-deprived and stressed is a body that is hormonally primed for insulin resistance. Prioritizing seven to nine hours of sleep and building in genuine recovery time is not a luxury... it is part of the treatment.
Medication may be recommended.
For some women, lifestyle changes alone are not enough, or the condition has progressed to a point where medication provides important support. Metformin, the most commonly prescribed medication for insulin resistance and prediabetes, improves how cells respond to insulin and is often used alongside lifestyle changes... not as a replacement for them. For women with PCOS, Metformin may also help regulate periods and improve fertility outcomes.
Do not wait for a diabetes diagnosis to take insulin resistance seriously. If you are experiencing several of the symptoms described above, especially fatigue after eating, belly weight that won't budge, irregular periods, brain fog, or dark skin patches... it is worth asking for a metabolic evaluation now, not later.
The earlier insulin resistance is identified, the easier it is to address. And in many cases, catching it early means you may never progress to prediabetes or type 2 diabetes at all.
A telemedicine consultation with 800Zed is a practical first step. You can discuss your symptoms with a doctor from home, find out which tests to request, and get a clear picture of where your metabolic health stands. If a physical examination or follow-up is needed, a clinic visit or home visit can be arranged wherever you are in the Philippines.
Your body has been giving you signals. Now is a good time to listen.
Book a consultation with 800Zed today: https://800zed.com
Arden Endocrinology Clinic. Insulin Resistance in Females: Key Symptoms Explained. September 2025.
American Diabetes Association. Understanding Insulin Resistance. May 2024.
Cleveland Clinic. Insulin Resistance: What It Is, Causes, Symptoms and Treatment. September 2023.
Arden Endocrinology Clinic. How to Manage Insulin Resistance with Diet and Exercise. November 2025.
MD Anderson Cancer Center. What's the Best Diet for Insulin Resistance? February 2025.
UCLA Health. Insulin Resistance Can Be Helped with Diet and Exercise.
PMC / NIH. Hyperglycemia and Type 2 Diabetes Among Filipino Women.
We use cookies to give you the best service on our site. By continuing to use the site you consent to our Privacy Policy
📲 Install 800 ZED App for quick access!
📲 Install 800 ZED App on your iPhone
Tap Share → Add to Home Screen
📲 Install 800 ZED on Firefox
Open menu ☰ → Install
Subscribe our newsletter for latest updates
Get the latest updates, promotions, and news delivered straight to your inbox.